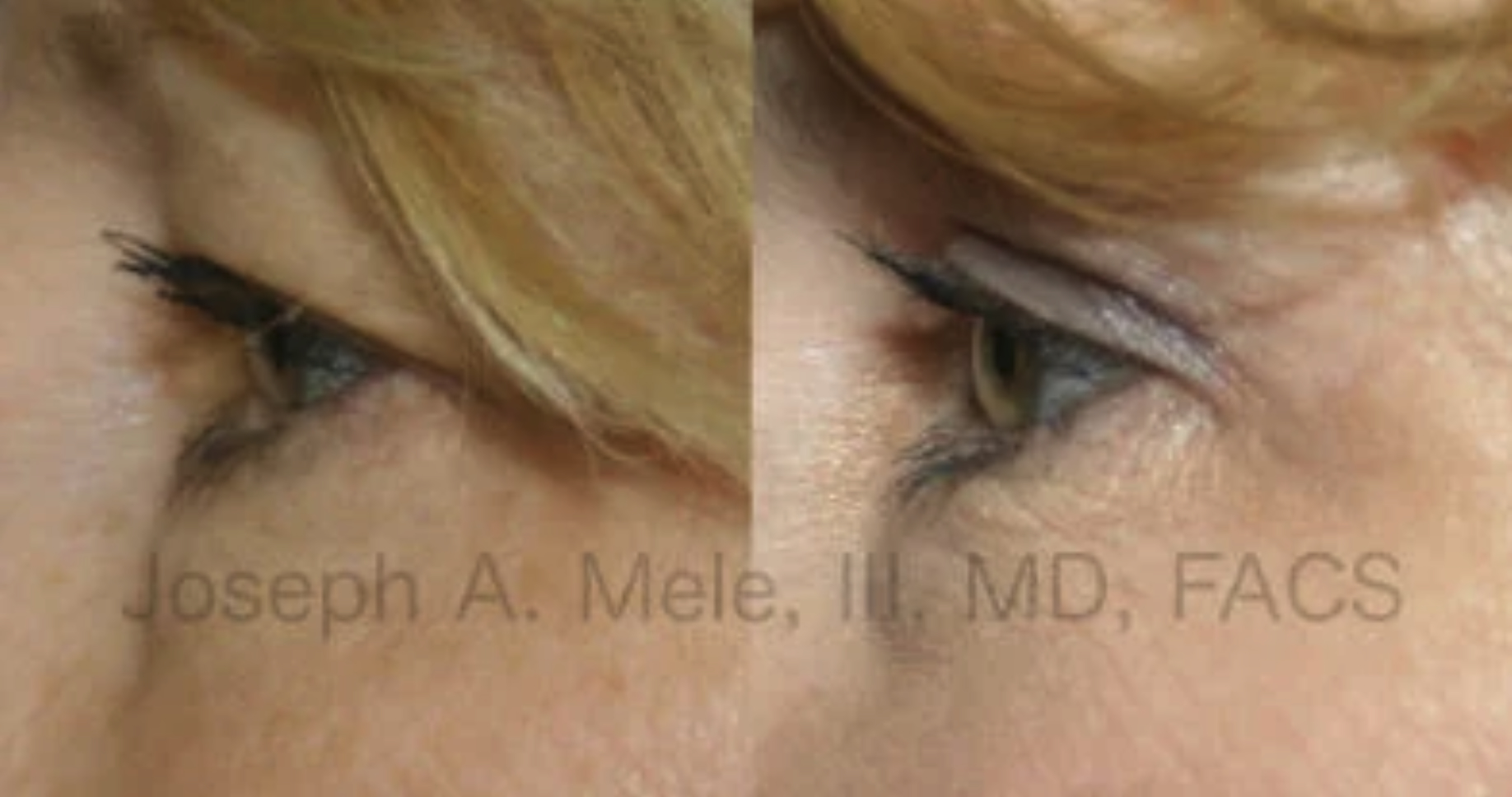
What Can Blepharoplasty Do For Your Eyelids?
Many patients come to my office looking to improve their facial aesthetics. A major area for rejuvenation is the eyelids. Heavy upper eyelids and […]
CDC Warns: Counterfeit Botox has Reached the United States
According to the Centers for Disease Control and Prevention (CDC), “As of April 12, 2024, a total of 19 people from 9 states have […]
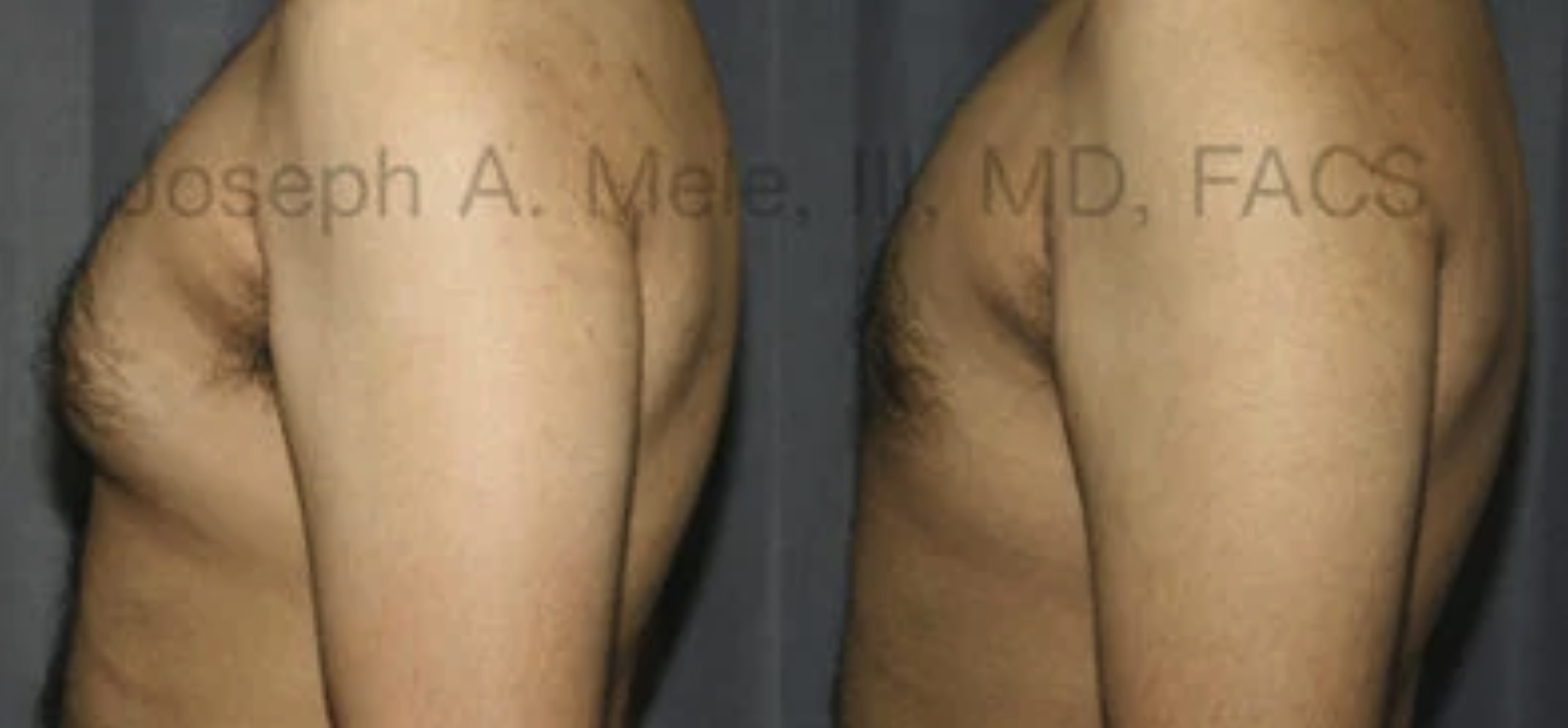
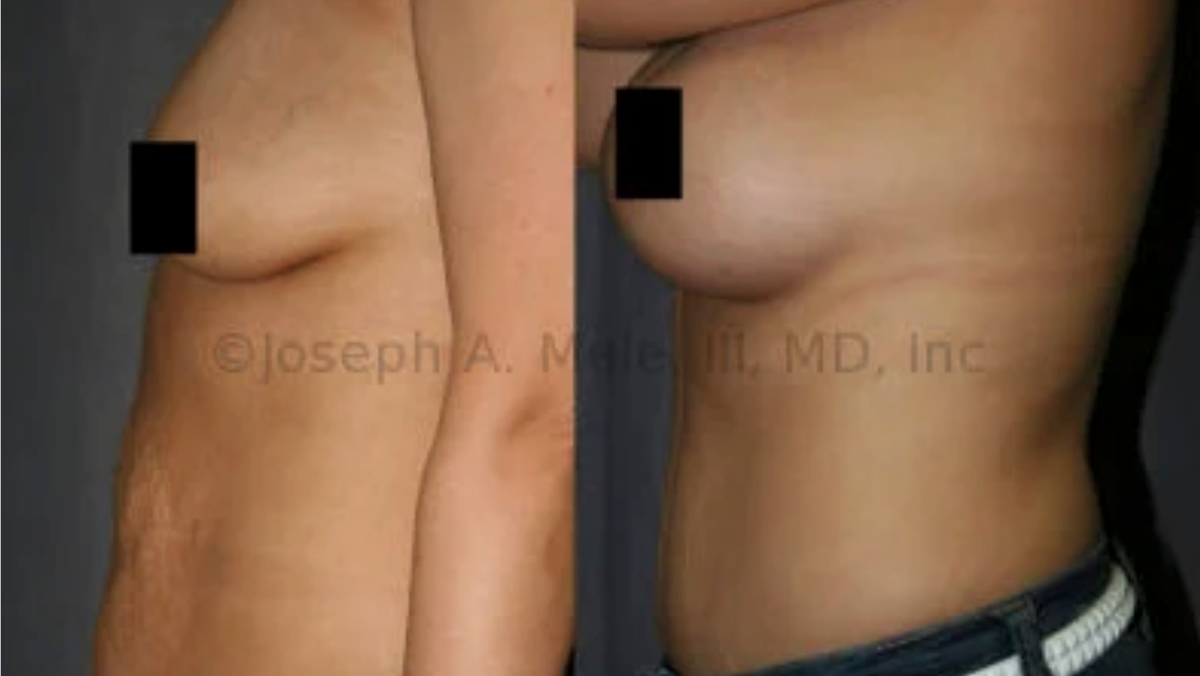
Twenty-Five Years of Masculinizing the Male Chest
I have been fortunate to practice Cosmetic Plastic Surgery in the San Francisco Bay Area for over 25 years. Like most plastic surgeons, the […]
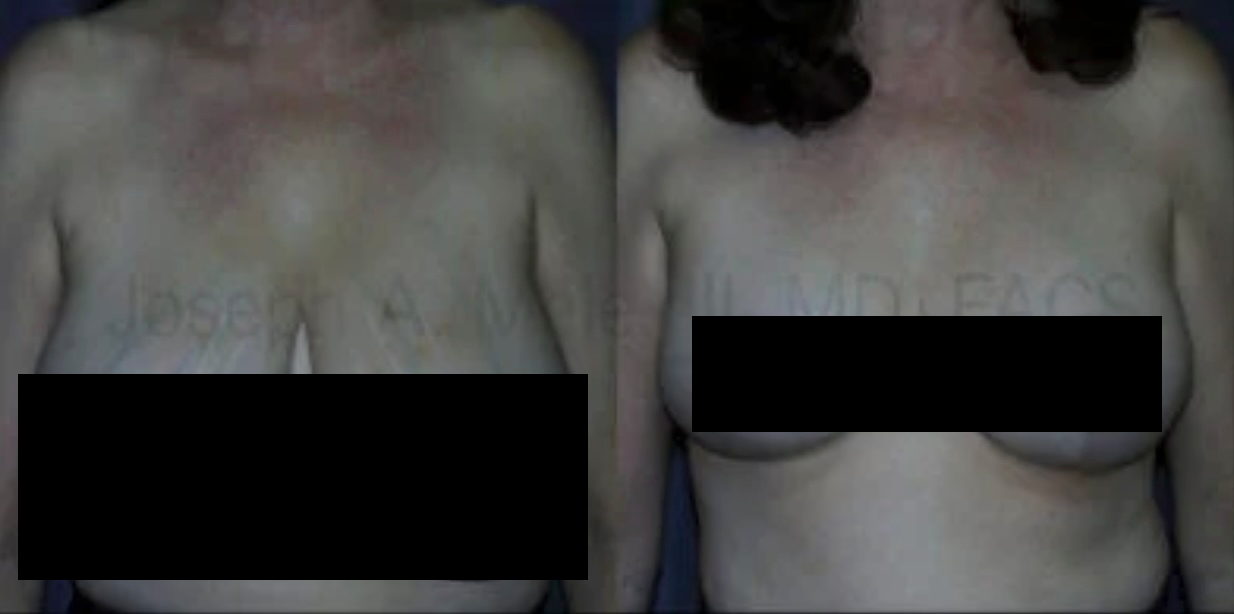
What Can Breast Reduction Do For You?
Breast Reduction for Women remains one of the most requested plastic surgery procedures in the US. It is third in line after Breast Augmentation […]
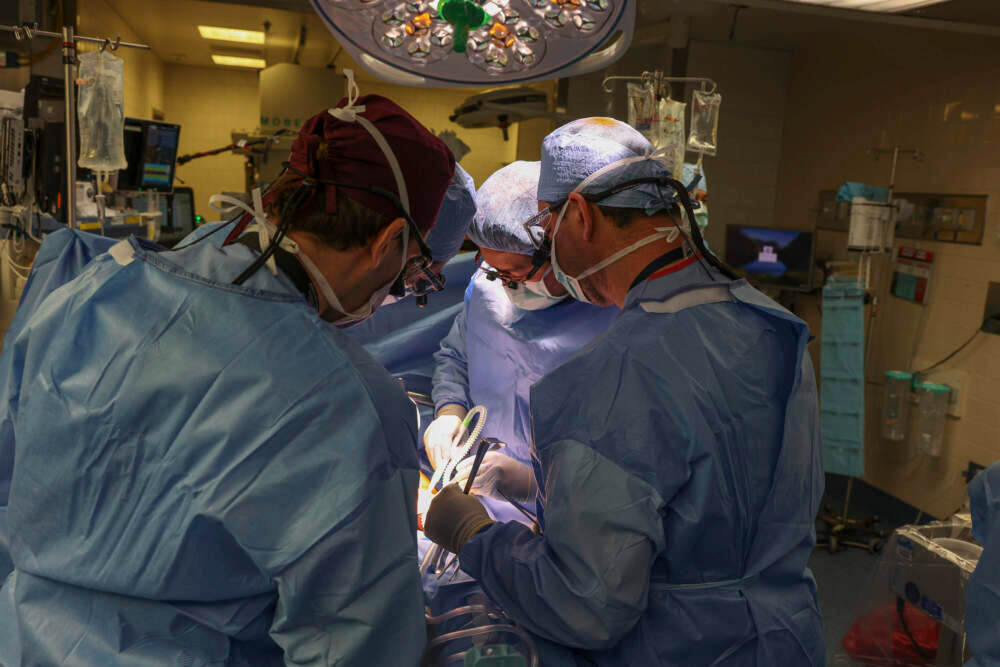
First Kidney Transplant From Pig to Human
The first kidney transplant was performed in 1954. It was the first human organ to be successfully transplanted. The achievement ushered in an era […]
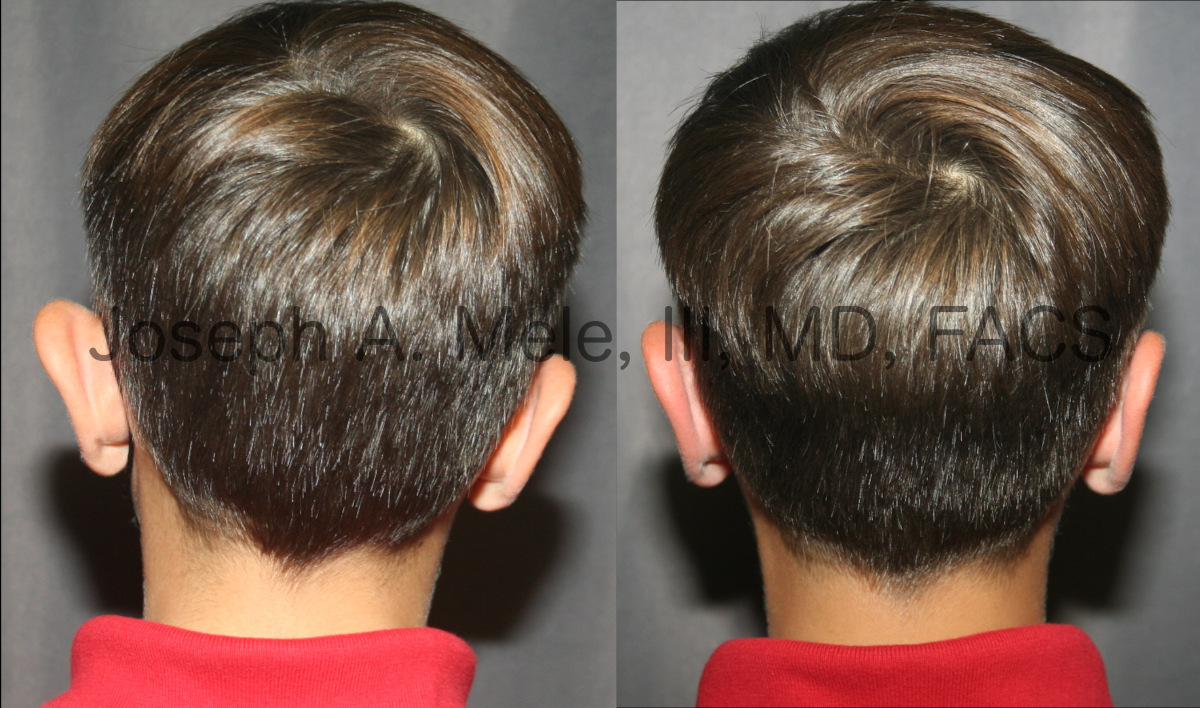
Ear Pinning For Prominent Ears – Otoplasty Pearls
Otoplasty is a category of Cosmetic Ear Surgery that includes Ear Pinning for Prominent Ears and the correction of other ear shapes like Cupped […]
Tummy Tucks – What Are They and What Do You Need to Know
The Tummy Tuck or Abdominoplasty is one of the most frequently performed cosmetic plastic surgery procedures. Abdominoplasty literally means abdomen changing, and changing the […]
Your 2024 Talk Awards Winner – Dr. Joseph Mele of Walnut Creek
For its dedication to providing excellent patient service, Joseph A. Mele, MD, FACS – Plastic Surgery of Walnut Creek, California, has won The Talk […]
2024 Aesthetic Everything Award Winner – Plastic Surgeon Dr. Joseph Mele
The 2024 Aesthetic Everything Awards are out. Thank you to everyone who voted over the last month, and your votes have been counted. I […]
Top 10 Plastic Surgeon Award for 2024 – and your chance to vote for more.
It is awards season, and Excellence in Plastic Surgery is also recognized. I am happy to report receiving the NAOPS’s Top 10 Plastic Surgeon […]