In response to questions asked about the case study of capsular contracture previously posted, I am expanding the information into a short three part mini-series on San Francisco breast augmentation revision surgery (click for Part 1) and capsular contracture in general. Part 1 is the breast implant revision surgery case study. Part 2 is this posting with more information about what capsular contracture is. Part 3 will be about the prevention on treatment of capsular contracture.
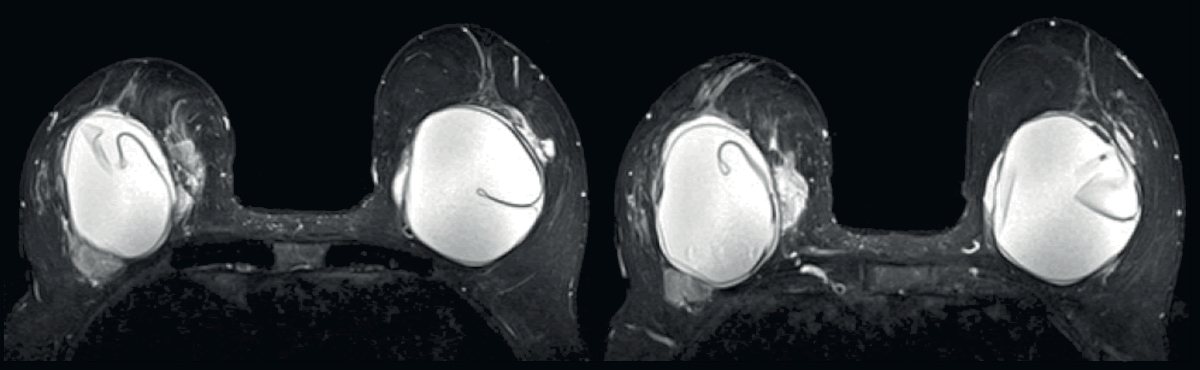
Capsular contracture on MRI with rupture and silicone extravasation.
Capsular contracture, or tightening of the scar that contains the implant, accounts for about one third of all breast augmentation revisions. According to the American Society of Plastic Surgeons, it is second only to a desire to change sizes. What is capsular contracture? How can it be prevented? How is it treated? San Francisco breast augmentation revision patients want to know.
It is desirable that a scar form around the breast implant. The scar, which forms the pocket that the breast implants sits in, is called the capsule. The capsule is very important.
If no scar, or a very weak scar forms, the implant is more likely to migrate. Gravity can pull the implant down (call bottoming-out) or the natural curve of the ribs can cause the implants to move laterally to the axilla (the armpits). The implants can also move together causing symmastia (connected breasts). A good capsule helps to secure the implants in their desired position, and helps maintain the desired results.
Capsular contraction occurs when the scar in the capsule is too tight or too thick. While Wikipedia defines capsular contracture as an abnormal response of the immune system, it is more likely an exaggerated normal response. If it is tight all around the implant, it can make the breasts feel hard and immobile. If it is tight on just one side, it can push the implant. For example, when the scar is tight on the bottom, it moves the implant up. This is the opposite of bottoming out.
*Capsular contracture is graded (Baker Grades) as follows:
- Grade I-Naturally soft. Not palpable
- Grade II-Increased firmness. Scar is palpable. No visual distortion.
- Grade III-Firm to touch. Immobile causing visual distortion.
- Grade IV-Same as Grade III and painful.
Grades I and II are the most frequent results and are not usually treated. Grades III and IV are less frequent, and are often treated with a revision breast augmentation.
Previous Post Next Post