Can Blood Tests Detect Cancer Earlier than Current Methods?
Blood Tests can detect cancer earlier than some current methods by identifying specific biomarkers, like circulating tumor DNA (ctDNA), proteins or exosomes, often before […]
Does Warming Patients During Surgery Improve Wound Healing?
It has long been asserted that cold patients have more wound healing problems, but what does the science say? A recent article in the […]
ASPS statement on Gender-Affirming Surgery for Adolescents
The American Society of Plastic Surgeons (ASPS) is the first major American medical body to oppose gender-affirming surgeries for minors. This is not a […]
Marijuana Use and Plastic Surgery. How Bad is Cannabis?
I find it ironic, and sad, that one week after two major studies showing the significant health risks of smoking marijuana and the dangers […]
Hello Nasal Epinephrine Delivery and Goodbye to the Needle
The FDA has been busy this month. Last week they advised on The Dangers of Skin Peels Without Professional Supervision. This week, the Food […]
The FDA Says Skin Peels Without Professional Supervision are Dangerous
The FDA just issued a new warning to consumers about do-it-yourself home chemical peels. Their advice, like President Biden’s is, “Don’t.” Do not purchase […]
American Board of Plastic Surgery Continuous Certification
“The Mission of the American Board of Plastic Surgery Inc., is to promote safe, ethical, efficacious plastic surgery to the public by maintaining high […]
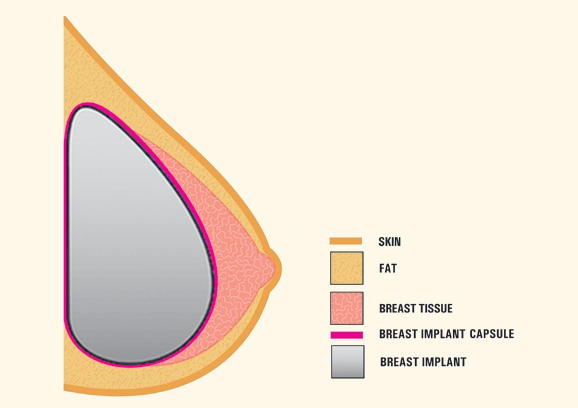
Statement on Breast Implant Capsulectomy Definitions 2024
Surgical treatment of breast implant capsules are varied and diverse. Today, I want to review the available options and outline when they are used. […]
2024 Aesthetic Everything Awards Voting is Open – Vote Now!
Voting for the 2024 Aesthetic Everything Awards is open. You can vote for your Favorite Plastic Surgeon, every day, now through February 7. Last […]
What’s Wrong With Daylight Saving Time?
This weekend we all enjoyed an extra hour as we fell back to standard time. Many doctors, however, are not fans of daylight savings […]