My surgical oncology professor, Dr. James E. Goodnight, of the University of California, Davis Medical Center, used to say,”Melanoma is the tumor that gives cancer a bad name.” Melanoma is the most deadly form of skin cancer. While it accounts for only 2% of all skin cancers, it is responsible for the majority of skin cancer deaths. 70,000 new cases of melanoma are diagnosed each year, with a projected 9,000 deaths.
Typical Melanoma
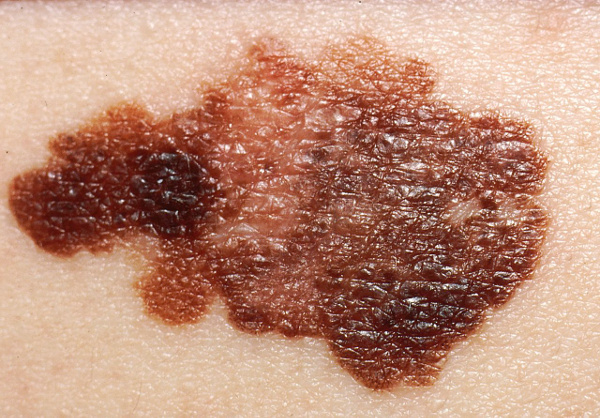
The Typical Melanoma has: A) Asymmetry; B) Borders that are irregular and not smooth; C) Colors that vary from red, white to blue; D) Diameter that is increasing in size. These are the ABCD’s of melanoma.
Prevention is the Best Medicine
While melanoma treatment has come a long way, the incidence of melanoma is going up, according to data presented this week at the annual meeting of the American Society of Clinical Oncology. Over the past 40 years, the incidence of melanoma among U.S. children and young adults has increased over 250%. Young women are particularly vulnerable, despite nation-wide educational efforts to increase awareness of the dangers of UV exposure.
Tanning beds and Skin Cancer Go Hand-In-Hand
According to the FDA, anyone who uses a tanning bed before age 35 increases their lifetime risk of melanoma by 75%. Young patients who use tanning booths more than ten times a year increase their risk of melanoma seven fold. Moreover, UV exposure also increases the risk of squamous cell carcinoma, the second most deadly skin cancer by two and a half times, and the risk of basal cell carcinoma of the skin by one and a half times. In addition to the increased risk of cancer, tanning is associated with premature aging, immune suppression, eye damage and allergic reactions. This has sparked many states to restrict the use of tanning beds for minors, a movement that has more recently become international.
There is No Such Thing as a “Safe Tan”

Whether you get your UV exposure from the Sun or a tanning bed, there is no such thing as a safe tan. Sun protection is a must. The umbrella would do more good shading her body than shading her possessions.
All tans, whether from the sun or a sun bed, are bad; however, sunburns are even worse. As few as five blistering sunburns as a child is associated with and increased incidence of melanoma, squamous cell carcinoma and basal cell carcinoma. The risk of melanoma continues to rise with an increasing number of sunburns. This is true for children, adolescents and adults.
Other Melanoma Risks
There are several risk factors for melanoma including:
- Excessive ultraviolet (UV) light exposure – Natural sun or otherwise
- A history of sunburn – Even just one
- Fair skin – Less pigment = less protection, especially if you can’t tan
- Lighter hair color – The lighter the worse
- Living closer to the equator – Less atmospheric refraction
- Living at a higher elevation – Less atmospheric diffusion
- Having many moles or unusual moles
- more than 100 “normal” moles increases the risk
- more than 10 “normal” moles on your arms increases the risk
- moles greater than 10 mm in diameter
- multicolored or irregularly shaped moles
- A family history of melanoma – more family members and more closely related family members
- Weakened immune system – immunosuppressive drugs or diseases
- Increasing Age – Older then 55
- Male Gender – sorry guys
- Previous melanoma – 8-12% melanoma patients have more than one
- History of Breast Cancer – may be due to a weakened immune system
What to Look For
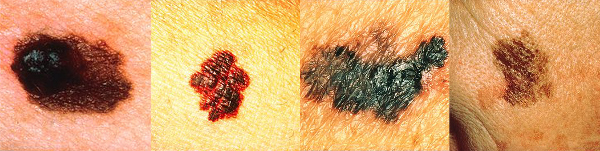
Each melanoma above depicts a typical finding. From left to right they are:
A) Asymmetry; B) Borders that are irregular and not smooth; C) Colors that vary from red, white to blue;
D) Diameter that is large or increasing in size.
90% of melanomas can be cured, and the key is early detection and treatment. A yearly full body check with a Board Certified Dermatologist is recommended for anyone with an increased risk for skin cancer. Self examination can help, if you know what to look for. Seek care from a dermatologist or your family doctor for moles with any of the following:
- Bleeding or itching
- Irregular border
- Change in shape or color
- Increase in size
- New mole or freckle
Not All Melanomas Are Black!
As if melanoma was not evil enough, 5% of melanomas are “amelanotic”, or without pigmentation. These are the toughest to diagnose, and can give even experienced doctors trouble. Unlike their darker cousins, amelanotic melanoma can look very bland.
Sunscreen Season
Though we Californian’s will have less water for our pools this summer, the sun will still be shining. Be certain to wear sunscreen, and avoid excess sun whenever possible. And if any of your moles are growing or changing, be certain to get them checked out.
Previous Post Next Post