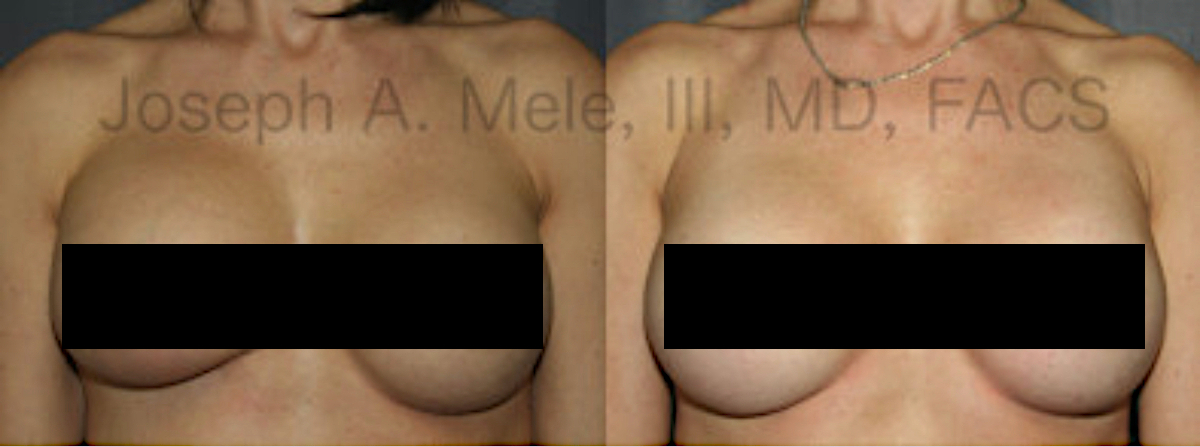
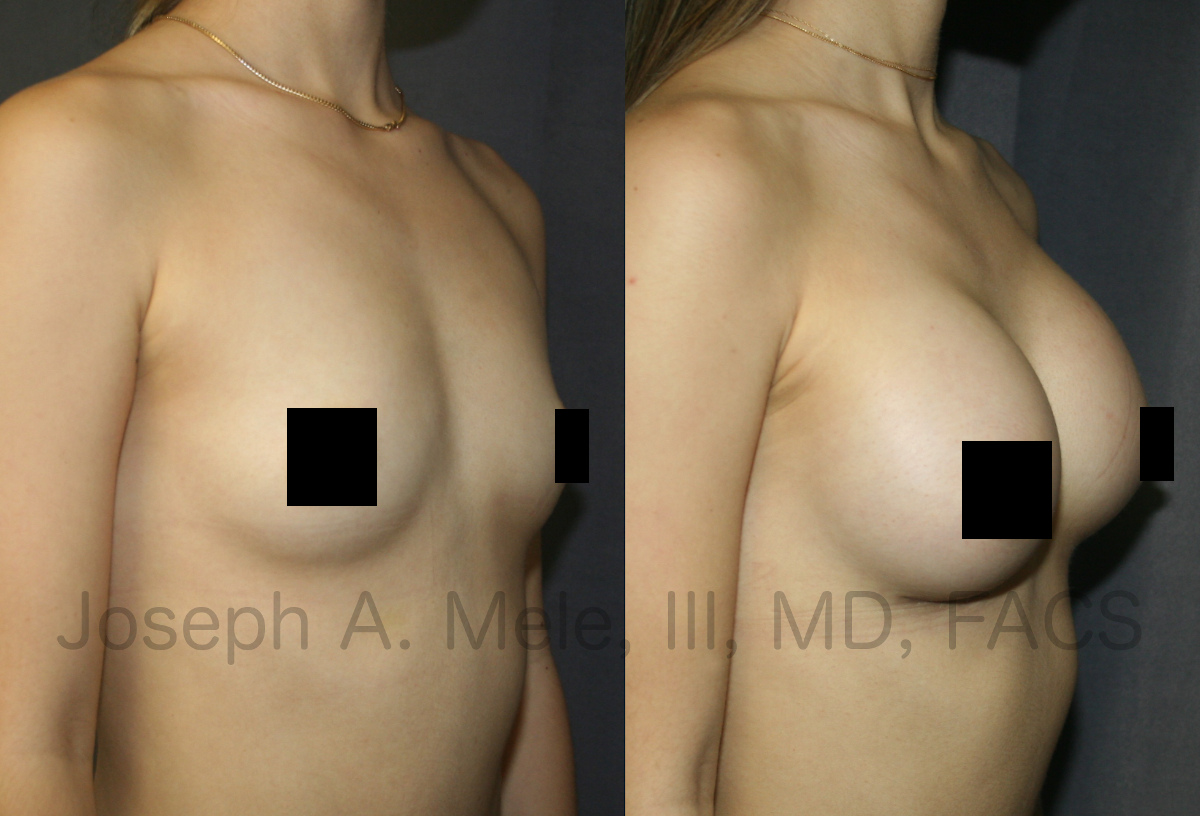
Top 10 Breast Augmentation Frequently Asked Questions
Today, we review the Top 10 Frequently Asked Questions about Breast Augmentation. These questions come from my patients and from inquiries on sites like […]
Top 10 Mommy Makeover Frequently Asked Questions (FAQs)
The Mommy Makeover remains one of the most commonly performed Cosmetic Plastic Surgery Procedure combinations in the San Francisco Bay Area. Today, on the […]
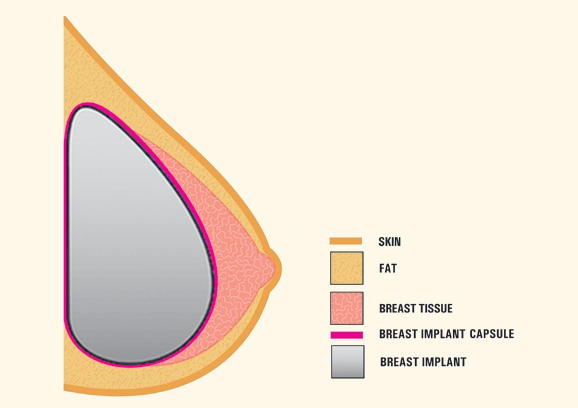
Statement on Breast Implant Capsulectomy Definitions 2024
Surgical treatment of breast implant capsules are varied and diverse. Today, I want to review the available options and outline when they are used. […]
Downsizing Breast Implants – What You Need to Know
Breast Augmentation remains the most popular elective cosmetic plastic surgery procedure and has one of the highest patient satisfaction ratings. The ability to provide […]
Breast Augmentation Options Breast Implants and Fat Grafting
Breast Implants have been around for 60 years, and Fat Grafting to the Breasts even longer. While Breast Augmentation with Breast Implants quickly, and […]
Breast Implant Maintenance and Breast Revision Surgery
Breast Augmentation Revision is used to maintain the aesthetic results of breast enhancing surgery. As we discussed last week, Breast Implants are not lifetime […]
Breast Implant Maintenance and Breast Revision Surgery
Breast Implants have come a long way over their 60 years of existence. They are available in a wider range of shapes, volumes and […]
Why Choose Breast Augmentation Near Me?
Breast Augmentation continues to be one of the most frequently requested cosmetic plastic surgery procedures. While Breast Implants have changed, the goals of Breast […]
Breast Implant Replacement Surgery
A week doesn’t go by without someone asking, “When do I need to replace my breast implants?” The simplest answer is, “When there’s a […]
Happy Patient = Happy Plastic Surgeon
It is an honor and a blessing to be a plastic surgeon. I get to practice medicine, one of the most challenging and stimulating […]